Key Takeaways
-
- When evaluating an Endocrinology EHR system, consider factors beyond the initial cost.
- The true expense of a low-cost EHR manifests in inefficiencies, staff burnout, compliance challenges, and decreased patient satisfaction.
- A comprehensive, scalable EHR may require a larger upfront investment, but it ultimately enhances workflow efficiency, elevates patient care, and mitigates the risk of incurring additional costs from hidden fees.
- Explore 5 strategies for a seamless endocrinology EHR transition.
At first glance, a budget-friendly EHR might appear to be the ideal choice for an expanding endocrinology practice. After all, why invest more when an “affordable” option is available? However, many practices soon realize that what seems economical on the surface often leads to frustration, unexpected costs, and significant workflow interruptions.
If you’re considering options like a low-cost EHR for Endocrinology practices or even pondering, “is there a free EHR?”, it’s crucial to grasp the complete scope of what you’re actually investing in.
Let’s delve into the hidden costs associated with adopting a system that only appears to be budget-friendly.
Table of Contents
The True Cost of Implementation
Implementation often reveals the first wave of unexpected costs. With many low-cost EHRs, onboarding is usually minimal, offering little more than basic guidance. This results in:
- Inadequate training that leaves staff uncertain about how to utilize the system effectively
- Increased time spent troubleshooting rather than focusing on patient care
- Additional fees for “premium” training sessions or extended support
For endocrinology practices, this can be particularly disruptive. Picture your team struggling to document follow-ups for diabetes management or thyroid function tests without the appropriate templates. Instead of concentrating on patient care, they waste hours trying to adapt a generic system to their needs.
Established vendors like Endocrinology-Cloud tackle these issues by offering free implementation and extensive, tailored training designed specifically for endocrinology workflows.
Workflow Disruption: The Hidden Cost
- Documentation delays: endocrinology providers frequently require specialty-specific templates for lab results, medication management, or patient education. Generic systems force providers into time-consuming manual processes.
- Inefficient billing processes: Shortcomings in revenue cycle management, such as missed codes for lab tests or medication refills, can lead to claim denials.
- Staff burnout: Excessive clicks, repetitive data entry, and disrupted workflows consume valuable clinical time and contribute to high turnover rates.
Every minute lost navigating a poorly designed system is a minute not spent with patients. Those “lost minutes” directly correlate to lost revenue and a decline in the quality of care provided.
The Hidden Costs: Add-Ons and Fees
Many endocrinology practices begin with a low initial price, only to discover that essential features are locked behind additional fees. Common examples include:
- Advanced reporting or analytics (e.g., to monitor treatment outcomes)
- Customization of templates and forms for endocrinology-specific procedures
- Secure messaging or patient portal access
- E-prescribing, particularly for controlled substances
What initially appeared to be an affordable EHR for endocrinology practices can rapidly escalate into a system that costs more than premium alternatives—without delivering equivalent value.
Telehealth and Fragmented Charges
In today’s healthcare landscape, telehealth is essential for ensuring patient access. However, with a low-cost EHR, you may find that telehealth capabilities are offered as expensive add-ons or, worse, are entirely unavailable.
For endocrinology clinics, managing multiple systems for patient follow-ups, post-operative consultations, and routine care can be a daunting task. This fragmentation not only leads to increased subscription costs but also heightens compliance risks and diminishes overall operational efficiency.
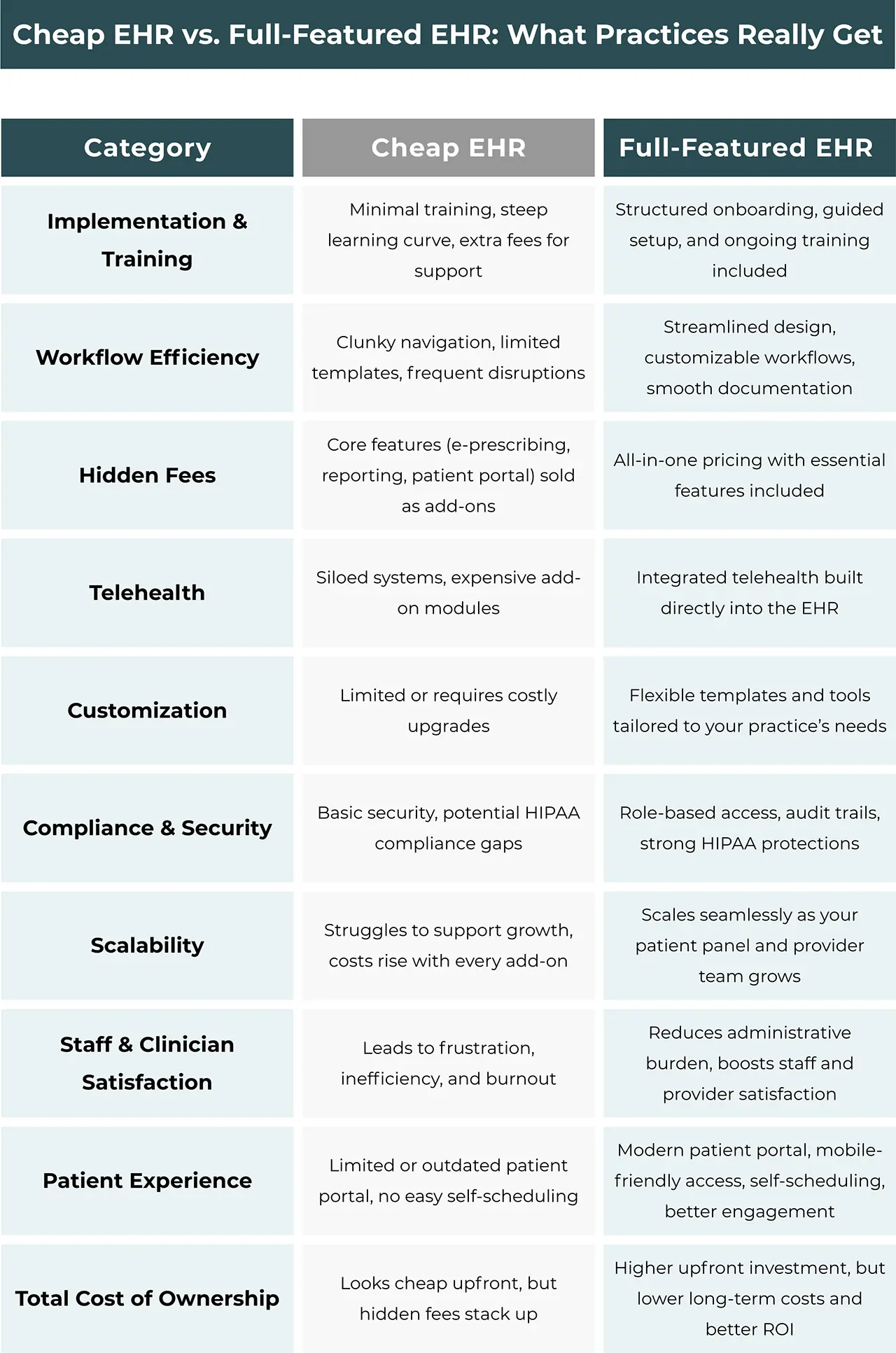
How Much Does an Endocrinology EHR Cost, Really?
Determining the cost of an endocrinology EHR involves more than just the initial price tag; it requires a thorough understanding of the total cost of ownership (TCO):
- Direct costs: Licensing fees, setup expenses, ongoing support, and training
- Indirect costs: Decreased staff productivity, patient no-shows, billing inaccuracies, and turnover due to clinician burnout
- Growth costs: Additional fees for every new provider, feature, or integration required as your practice expands
What a Full-Feature EHR Provides From Day One
In contrast to limited systems that require you to navigate complexities on your own, a comprehensive endocrinology EHR is designed to support your success from the outset. This includes:
- Free implementation support – Endocrinology-specific workflows, templates, and settings are configured correctly from day one, ensuring a smooth start.
- Comprehensive training – Proper training leads to an impressive 83% satisfaction rate among end-users, compared to just 36% for those without it.
- Data migration included – Seamless transfer of patient records, demographics, and historical notes without incurring additional costs.
- Practice-specific customization – Tailored templates for endocrinology care streamline processes and enhance efficiency.
- Ongoing support at no extra charge – Access to responsive customer support and continuous training keeps your staff informed and capable.
The distinction is evident: rather than facing incremental charges for essential services, you gain a partner dedicated to your long-term success.
Choosing Wisely: Invest in Long-Term Value
Instead of inquiring, “Is there a free EHR available?”, consider asking:
- Will this system scale as my endocrinology practice expands?
- Does it offer specialty-specific tools tailored for endocrinology care?
- Are telehealth capabilities, patient engagement features, and reporting functionalities included or sold separately?
- What level of support and training is provided?
While an inexpensive EHR may seem appealing at first glance, the hidden costs associated with implementation challenges, workflow disruptions, add-ons, and separate telehealth fees can gradually deplete your practice’s resources.
Investing in a robust EHR specifically designed for endocrinology practices is more about value than mere cost. The right solution not only supports your growth but also enhances clinician satisfaction and ensures that patients receive the quality care they deserve.






